 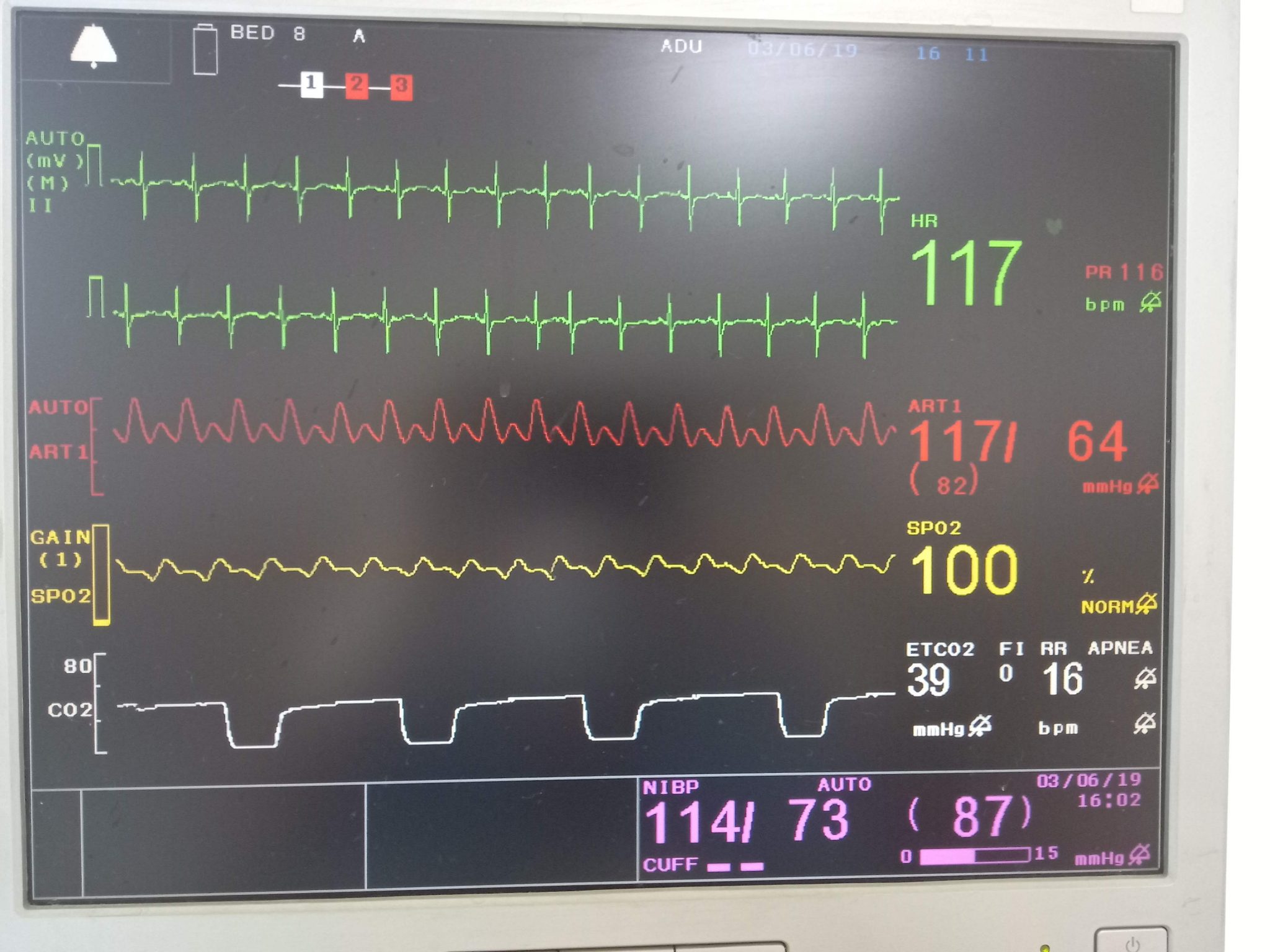
Phase I does not contain any expired carbon dioxide (dead space gases, zero PCO 2). 1C), based on the physiology of carbon dioxide evolution from the lungs and airways. 4–6The expiratory segment is further divided into three phases (I, II, III), and an occasional phase IV ( fig. A time capnogram has two important segments: inspiratory (phase 0) and expiratory. Time capnography is used more commonly in clinical practice. 1A) or expired volume (volumetric capnogram, fig. Carbon dioxide waveforms can be plotted against time (time capnogram, fig. Any variation from this requires an analysis to determine a physiologic or pathologic cause of the variation. 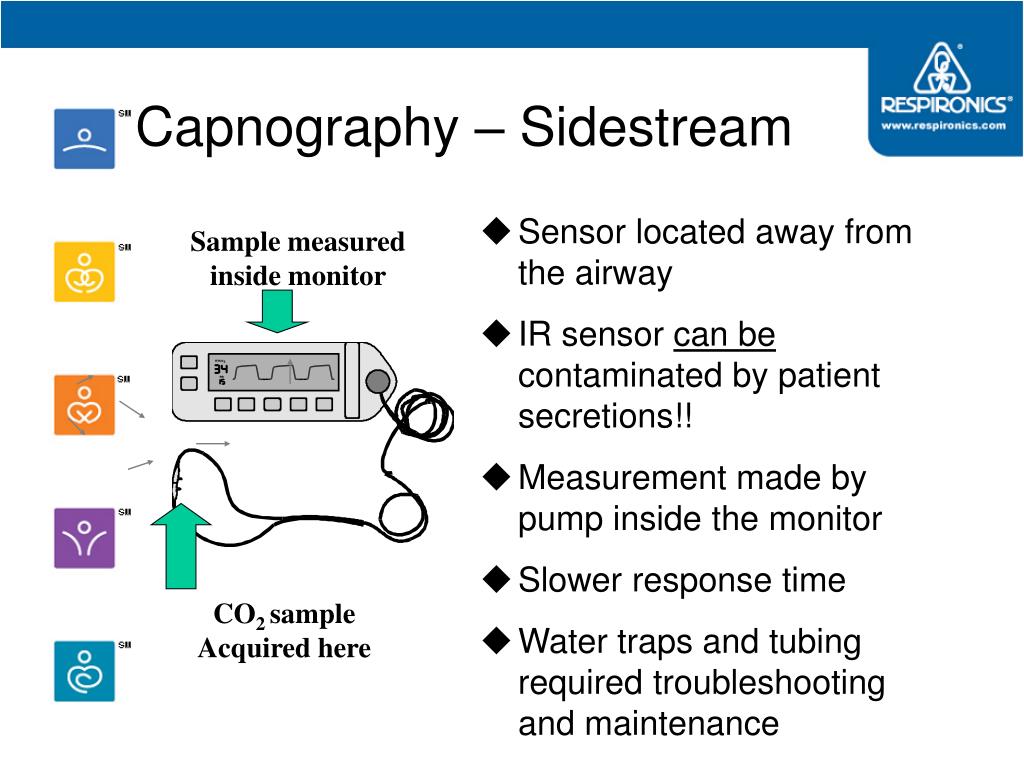
The transport of gases to the infrared measuring device results in a delay of 1–4 s in carbon dioxide measurement and display of capnograms in sidestream capnography.Ī conventional capnogram in adults results in a more or less identical shape in all healthy individuals. In sidestream technology, the respiratory gases are aspirated via an adaptor and a 6-foot sampling tube to the monitor housing the infrared sensor. In mainstream sensors, the adaptor housing the sensor is interposed between the tracheal tube and breathing circuit, and the measurement of carbon dioxide is made across the airway. Depending on the location of the carbon dioxide measuring device, there are two sensor types: mainstream and sidestream. 3The carbon dioxide values are usually displayed as partial pressure (PCO 2). Efforts have been made to decrease the response time and increase the accuracy of infrared technology to produce superior capnography waveforms even in premature babies with small tidal volumes and rapid respiratory rates. Infrared technology is by far the most common and cost-effective method of carbon dioxide measurement and monitoring. 1, 2This “Clinical Concepts and Commentary” will summarize physiology and clinical interpretation of capnography and update the current status of capnography outside of the operating rooms, including public and media awareness, and suggest probable future directions. Nonetheless, in the last 2 yr there has been a surge in understanding and recognizing the value of capnography outside of the operating rooms. One of the obvious reasons seems to be a lack of a single society overseeing the safety of outside-the-operating-room procedures the way ASA and AAGBI do in the operating room. However, in many institutions, capnography is not used to monitor ventilation during sedation for procedures performed particularly by nonanesthesiologists outside of the operating rooms. As anesthesiologists, we use capnography to monitor sedation in the operating room because we appreciate that the line between consciousness and unconsciousness is very thin, and the patient can drift from one state to another. It is even more surprising that many ICUs do not have capnography either to confirm endotracheal intubation or to continually monitor ventilation. It is not uncommon in our practice to observe an intubated and ventilated patient, originally monitored with capnography in the operating room, but then transported to the intensive care unit (ICU) without capnography. Although capnography has become an integral part of anesthesia care in operating rooms for more than 25 yr, its value has been limited to these situations and is not well appreciated beyond these confinements. Capnography is mandatory for laparoscopic surgeries for reimbursement). Currently, anesthesiologists in many developing countries follow these recommendations (India, Government of Andhra Pradesh Order, AST/775/F25/dated September 2011. Thanks to the foresight of the American Society of Anesthesiologists (ASA), Anesthesia Patient Safety Foundation (APSF), Association of Anaesthetists of Great Britain and Ireland (AAGBI), and the Association of Anesthesiologists in Holland, capnography was embraced and incorporated into the standards of monitoring during anesthesia to enhance patient safety. Such a decrease has not been seen in other medical or surgical specialties over this time frame. In the United States, since 1985, there has been a dramatic decrease in the malpractice insurance premiums of anesthesiologists. HISTORICALLY, anesthesiologists seem to be the forerunners in implementing tools and standards for safety in the medical fraternity. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
